Table of Contents >> Show >> Hide
- Quick Safety Check Before You Chase the Pop
- What That “Crack” Usually Is (and What It’s Not)
- Why Your Upper Back Gets Stiff in the First Place
- Way #1: Foam Roller Thoracic Extension (The Classic, Controlled Pop-Opportunity)
- Way #2: Seated Chair Thoracic Extension (The Office-Friendly “I Still Have Meetings” Option)
- Way #3: Side-Lying “Open Book” Rotation (The Gentle Twist That Doesn’t Pick a Fight With Your Neck)
- How to Make Upper-Back Relief Last Longer Than a Coffee Break
- When You Should Get Professional Help
- FAQ: The Stuff Everyone Wonders but Rarely Googles Politely
- Real-Life Experiences Related to Cracking Your Upper Back (500+ Words)
- Conclusion: Crack Optional, Mobility Mandatory
Your upper back (a.k.a. the thoracic spine) can get so stiff that it feels like someone replaced your vertebrae with Legos.
And when you finally stretch, you might hear (or feel) that satisfying pop.
If you’re here because you want that “ahhh” moment without turning your living room into an amateur chiropractor’s office,
you’re in the right place.
This guide walks you through three safer, gentler ways to mobilize your upper backmethods that often
create a crack as a side effect, not a goal. Along the way, you’ll learn what the sound usually means,
when you should skip the DIY approach, and how to make the relief last longer than the length of a TikTok.
Quick Safety Check Before You Chase the Pop
A harmless crack is typically painless and followed by easier movement. But if cracking is your go-to coping strategy,
treat it like hot sauce: a little can be fine, but if you’re dumping it on everything, something else is going on.
Skip these techniques and get checked out if you have:
- Sharp pain (especially if it spikes with breathing, coughing, or movement).
- Numbness, tingling, weakness in your arms or legs.
- New balance problems or clumsiness.
- Fever, unexplained weight loss, or you feel unwell with the back pain.
- Recent trauma (fall, car accident, sports collision).
- New bowel or bladder control problems (urgent evaluation).
Also: if you have a condition that affects bone strength (for example, osteoporosis), a known spinal fracture,
or you’re recovering from surgery, get personalized guidance from a clinician before doing any “cracking” moves.
What That “Crack” Usually Is (and What It’s Not)
In many jointsincluding the small joints in your spinethe classic “crack” is commonly explained by
a pressure change inside a fluid-filled joint space. When you stretch or move a stiff joint,
the pressure shifts and dissolved gases can form a bubble, creating a popping sound (often called cavitation).
Translation: it’s usually not bones grinding and it’s not your spine “going back into place.”
You can also get noise from tendons or ligaments sliding over bony structuresmore like a quiet snap than a big pop.
Neither sound is automatically “good” or “bad.” The real win is improved motion, less stiffness, and no pain.
Why Your Upper Back Gets Stiff in the First Place
The thoracic spine is built for stability (it’s attached to your rib cage), but it still needs enough mobility to let
your shoulders move wellespecially if you reach overhead, lift, or spend hours hunched over a laptop like a modern-day gargoyle.
Common culprits include:
- Prolonged sitting with rounded shoulders and a forward head posture.
- Desk or phone time that keeps your upper back flexed for long stretches.
- Tight chest muscles and underused upper-back muscles (a classic push-more-than-you-pull problem).
- Stress breathing (shallow breaths can lock up the rib cage and upper back).
- Training patterns that skip mobility and thoracic extension (hello, bench press fans).
The best “upper back cracking” strategy is the boring one: restore mobility and build strength so stiffness doesn’t keep coming back.
But firstlet’s get you moving.
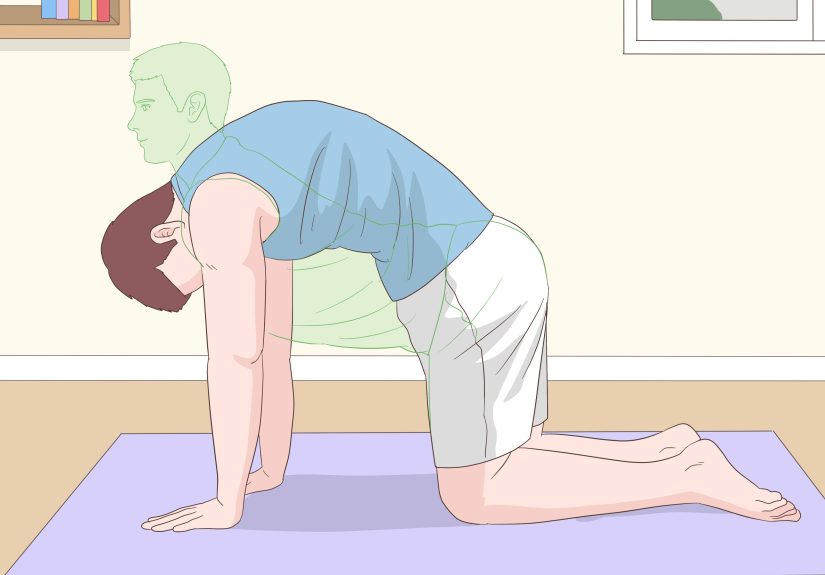
Way #1: Foam Roller Thoracic Extension (The Classic, Controlled Pop-Opportunity)
If your upper back had a “reset” button, it would look suspiciously like a foam roller. This move helps open up thoracic extension
(bending backward), which many of us lose with desk posture. It often produces a crackbut you’re aiming for smooth motion, not fireworks.
How to do it (step-by-step)
- Set up: Sit on the floor with knees bent, feet flat. Place a foam roller horizontally behind you.
- Position: Lean back so the roller sits across your upper back (around the shoulder-blade level), not your neck and not your low back.
- Support your head: Interlace fingers behind your head and keep elbows slightly in so your ribs don’t flare like you’re auditioning for a superhero movie.
- Brace gently: Lightly engage your core so the movement stays in the upper back, not the low back.
- Extend: Slowly arch back over the roller, inhale, and pause for 1–2 seconds in a comfortable stretch.
- Return: Come back to neutral. Repeat for 6–10 slow reps.
- Change levels: Scoot the roller an inch up or down and repeat, covering the mid-to-upper thoracic area.
Make it safer (and better)
- Move slowly. A slow, controlled extension tends to feel better and reduces the urge to “yank” on your neck.
- Keep it thoracic. If you feel pinching in the low back, reduce the range and tighten the core gently.
- No roller? Use a rolled towel or a firm pillow. Less “pop potential,” still helpful.
- Add breathing: Inhale into your rib cage as you extend; exhale fully as you return. Ribs love attention.
Common mistakes
- Rolling onto the neck and cranking your head back. Keep the roller on the upper back only.
- Hyperextending the low back to “fake” thoracic mobility. Smaller range, better target.
- Chasing cracks by bouncing. If you’re bouncing, your upper back is not getting smarterjust noisier.
Way #2: Seated Chair Thoracic Extension (The Office-Friendly “I Still Have Meetings” Option)
This is the move you can do between emails without anyone asking if you’ve joined a circus troupe.
It targets the same thoracic extension pattern as the foam rollerusing a chair back as the support.
Bonus: it’s easy to control and doesn’t require floor time.
How to do it
- Choose your chair: Use a sturdy chair with a mid-height back (not a wobbly bar stoolplease don’t make this your origin story).
- Sit tall: Feet flat, hips all the way back, spine long.
- Hands behind head: Support your head lightly; elbows point forward and slightly out.
- Find the fulcrum: Position the chair back against the mid-to-upper back (around the bottom of your shoulder blades).
- Extend: Gently arch back over the chair back. Keep your chin slightly tucked (think “make a double chin,” but politely).
- Breathe: Inhale into the ribs as you extend; exhale as you return.
- Repeat: 6–8 slow reps. Then shift the chair contact point slightly higher or lower and repeat.
Pro tips
- Keep your ribs down. If your rib cage flares aggressively, you’re borrowing motion from the low back.
- Pair it with a chest opener: After 1–2 sets, stand and do a gentle doorway chest stretch for 20–30 seconds.
- Use a towel: If the chair edge feels sharp, drape a towel over the chair back.
When it should NOT crack
If you’re moving smoothly and your upper back doesn’t pop, congratulations: you’re still doing it right.
Sound is optional. Mobility is the actual product you ordered.
Way #3: Side-Lying “Open Book” Rotation (The Gentle Twist That Doesn’t Pick a Fight With Your Neck)
A lot of “crack my back” attempts involve aggressive twistingoften through the neck or low back. The open book keeps things calmer.
It encourages thoracic rotation (turning) while your hips stay mostly stacked, which helps your upper back do its job.
How to do it
- Start position: Lie on your side with knees bent about 90 degrees, hips stacked, and arms straight in front of you (palms together).
- Anchor the knees: Keep knees together (you can place a pillow between them). The goal is rotation through the upper back, not your pelvis.
- Open up: Slowly sweep your top arm across your body, rotating your chest toward the ceiling and then toward the floor behind youlike opening a book.
- Let the ribs move: Breathe as you rotate; you’ll feel the rib cage and upper back expand.
- Pause: Hold the open position for 1–2 breaths, staying in a comfortable range.
- Return: Bring the arm back. Do 6–10 reps, then switch sides.
Make it more upper-back focused
- Keep the chin neutral. Follow your hand with your eyes, but don’t yank the neck.
- Exhale fully. A longer exhale can help the ribs soften and rotate.
- Small range is fine. You’re teaching your spine that rotation is safe, not trying to win an award for “Most Dramatic Stretch.”
If you feel it in the low back
Reduce the range, keep knees pinned, and try putting your feet on the wall for extra stability.
Low back grabbing usually means the thoracic spine is letting the lumbar spine do the work.
How to Make Upper-Back Relief Last Longer Than a Coffee Break
Cracking can feel great, but it’s often temporary if the underlying pattern doesn’t change.
The fix is usually a combo of mobility + posture habits + strength.
Think of cracking as clearing the browser cachenot rewriting the code.
Try these “movement snacks” (2–3 minutes total)
- Wall angels (8 reps): Back against the wall, ribs down, slide arms up and down slowly.
- Doorway chest stretch (20–30 seconds): Open tight pecs so shoulders can sit back where they belong.
- Shoulder blade squeezes (10 reps): Gently pinch shoulder blades down and back (no shrugging).
- Big breaths (5 slow breaths): Inhale into the ribs; exhale fully to reduce “stress armor” around the chest.
Strength moves that support a happier thoracic spine
- Rows (bands or dumbbells) to balance pushing volume.
- Face pulls for upper-back endurance and scapular control.
- Prone Y/T/W patterns for shoulder blade stability.
- Dead bug or similar core control work so your low back stops “helping” your upper back.
If you sit a lot, set a simple rule: every 45–60 minutes, stand up and do one minute of movement.
Your upper back loves consistency more than intensity.
When You Should Get Professional Help
If your upper back stiffness keeps returning, you’re cracking multiple times a day, or you’re getting pain (not just tightness),
it may be time for a real assessment. A physical therapist can identify whether you’re dealing with mobility restrictions,
muscle imbalance, breathing mechanics, shoulder limitations, or something else entirely.
A clinician may also help if your “tight spot” never seems to be the one that cracksa common scenario where a more mobile area
moves instead of the restricted one. (Your spine is clever like that. Sometimes too clever.)
FAQ: The Stuff Everyone Wonders but Rarely Googles Politely
Is it bad to crack your upper back?
Occasional painless cracking is generally considered common. The bigger issue is dependence:
if you need to crack constantly to feel “normal,” focus on mobility, posture habits, and strengthand consider getting checked out.
How often can I do these techniques?
For gentle mobility moves like these, many people do them daily or a few times per weekas long as they’re pain-free.
Start small (1–2 rounds) and see how your body responds over 24 hours.
Why doesn’t it crack anymore?
Sometimes there’s simply no cavitation at that moment. Also, the “pop” isn’t a measure of success. If your range of motion improves,
your shoulders feel freer, or you breathe more easily, you’re winningeven in complete silence.
What if I feel pain when I try?
Stop. Pain is useful information. Swap to gentler ranges, add heat, take a walk, and if pain persists or you have any red-flag symptoms,
seek medical advice.
Real-Life Experiences Related to Cracking Your Upper Back (500+ Words)
People talk about upper-back cracking the way they talk about peeling the plastic off a new phone: oddly satisfying, slightly addictive,
and sometimes a clue that something underneath needs attention. Here are common experiences many people report when they experiment with
upper-back “cracking” strategiesplus what tends to help the most.
1) The Desk-Job Crunch: “My Upper Back Feels Glued”
A classic story: you’ve been sitting for hours, shoulders drifting forward, chin reaching toward the screen like it’s trying to escape your body.
You stand up and your upper back feels stiffalmost “stuck.” When you try the chair extension or foam roller, you may feel a gentle stretch
across the chest and front ribs. Sometimes you’ll get a pop right away; other times the first few reps feel like you’re warming up rusty hinges.
People often say the biggest surprise is how much breathing changes the experience: a slow inhale into the side ribs makes the stretch
feel more targeted, and a full exhale makes rotation easier.
What tends to work best here is not a single dramatic crack, but a short routine done consistently:
one set of thoracic extensions, one doorway chest stretch, and a few shoulder blade squeezes. When people repeat that mini-sequence every day for a week,
they often report needing to “crack” less because the stiffness doesn’t build up as aggressively in the first place.
2) The Gym Pattern: “My Lats Are Tight, My Upper Back Won’t Extend”
Lifters often describe a different flavor of upper-back stiffness: they can pull heavy and press heavy, but overhead positions feel restricted.
During foam roller extensions, they may feel the stretch more in the sides of the rib cage (lats/serratus area) than directly on the spine.
Cracks may happen, but the bigger “win” is usually improved shoulder comfortespecially in overhead pressing or front rack positions.
People in this camp often learn a helpful lesson: if you chase cracks with aggressive twisting, the neck and low back tend to complain.
If you keep it controlledslow thoracic extensions, gentle open books, and some upper-back strength work (rows, face pulls)the stiffness usually
becomes less dramatic over time. In other words: you don’t need your spine to sound like microwave popcorn to make progress.
3) The Stress Armor: “I Hold Tension Between My Shoulder Blades”
Some people don’t sit that much, don’t lift that much, and still feel that tight, band-like tension between the shoulder bladesespecially during
stressful weeks. In these cases, the “need to crack” is often tied to muscle guarding and shallow breathing. The open book rotation can feel almost
emotional (yes, your rib cage is dramatic), because it combines movement with breath and a sense of decompression across the front of the chest.
The crack may or may not show up, but many people notice their shoulders drop away from their ears after a few slow reps.
A common experience here is that the relief fades quickly if you go right back into the same posture and stress pattern.
People often do better when they pair mobility with “downshift” habits: a short walk, a few slow exhales, and a posture reset at the desk
(screen higher, elbows supported, shoulders relaxed). The takeaway is simple: sometimes your upper back isn’t asking for a crackit’s asking for a
different day.
4) The “It Didn’t Crack, Did I Fail?” Moment
Many people try these moves and… nothing pops. The most common outcome? They still feel better. Less stiffness. Easier rotation.
A deeper breath. That’s your reminder that the crack is a sound effect, not the storyline.
Over time, people who focus on smoother motion and better posture habits often report fewer cravings to crack because their upper back simply
moves more easily throughout the day.
Conclusion: Crack Optional, Mobility Mandatory
If you want a safer path to upper-back relief, start with controlled thoracic extension (foam roller or chair) and gentle rotation (open book).
Move slowly, breathe, and stop if you feel pain. Then, make the results stick with quick daily posture breaks and a little upper-back strengthening.
Your thoracic spine doesn’t need more dramait needs better options.