Table of Contents >> Show >> Hide
- What Herniated Disc Surgery Is Actually Treating
- When Surgery Is Usually Considered
- Types of Herniated Disc Surgery
- How the Procedure Usually Works
- Risks and Possible Complications
- Recovery: What to Expect (Without the Sugarcoating)
- When to Call Your Doctor During Recovery
- FAQ: Quick Answers People Usually Want First
- Experiences People Commonly Report After Herniated Disc Surgery (Extended Section)
- Final Takeaway
If you are reading this while sitting in a very careful, very awkward position, welcome to the club. A herniated disc can turn ordinary thingslike tying shoes, driving, or sneezinginto dramatic events. The good news: most herniated discs improve without surgery. The even better news: when surgery is needed, modern procedures are often smaller, faster, and more targeted than many people expect.
This guide breaks down the main types of herniated disc surgery, what happens before and during the procedure, common risks, and what recovery actually looks like in real life. We’ll keep it practical, clear, and humanbecause spine jargon is not a personality trait.
What Herniated Disc Surgery Is Actually Treating
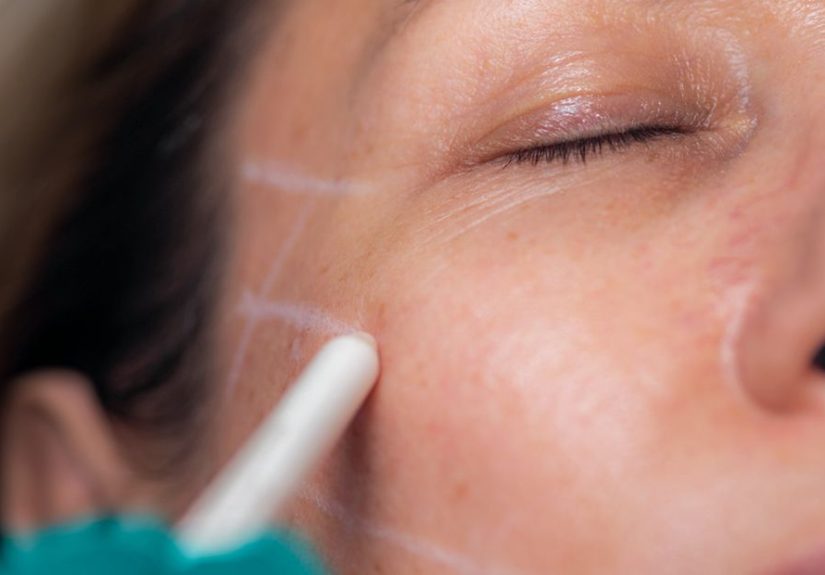
A herniated disc happens when the softer inner material of a spinal disc pushes through a crack in the tougher outer layer. That bulge or fragment can press on nearby nerves, which may cause pain, numbness, tingling, or weakness. In the lower back, this often shows up as sciatica (pain running down the leg). In the neck, symptoms may radiate into the shoulder, arm, or hand.
The goal of surgery is not to “fix every back problem.” It is usually to relieve nerve pressure caused by a disc herniation that matches your symptoms and imaging findings. That is why many surgeons focus on removing only the portion of disc that is compressing the nerve, rather than removing the entire disc.
When Surgery Is Usually Considered
One of the most important points: not every herniated disc needs surgery. In fact, many improve with time and conservative care such as anti-inflammatory medication, physical therapy, activity modification, and sometimes epidural steroid injections.
Surgery becomes a more serious option when one or more of these apply:
- Symptoms do not improve after a reasonable trial of nonsurgical treatment (often several weeks).
- Pain is severe enough to disrupt walking, work, sleep, or normal life.
- There is progressive weakness, numbness, or worsening neurologic symptoms.
- There are urgent warning signs such as bowel/bladder changes or severe neurologic deficits.
In plain English: if the disc is annoying, you usually start with conservative care. If it is crushing your quality of life or causing nerve damage, surgery moves higher on the list.
Types of Herniated Disc Surgery
“Herniated disc surgery” is an umbrella term. The actual procedure depends on where the herniation is (neck vs. lower back), how large it is, whether multiple levels are involved, and your anatomy.
1) Microdiscectomy (Microdiskectomy)
This is one of the most common procedures for a single lumbar (lower back) herniated disc. The surgeon uses a small incision and often a microscope or magnification to remove the herniated disc fragment pressing on the nerve.
Why it is common: it is targeted, effective for leg pain caused by nerve compression, and often less disruptive to surrounding tissues than older open approaches.
2) Standard or Open Discectomy
An open discectomy uses a larger incision and more direct exposure of the surgical area. It may still be the best approach in some situations, such as more complex anatomy, multiple levels, or when the surgeon needs broader access.
“Open” does not mean “bad” or “outdated.” It simply means the surgical exposure is larger. In some cases, that extra visibility is exactly what makes the procedure safer and more effective.
3) Minimally Invasive Discectomy
Minimally invasive discectomy (MIS discectomy) uses a smaller incision and specialized tools, often including tubular retractors and a camera or endoscope. The surgeon works through a narrow channel to reach the disc while minimizing muscle disruption.
Potential benefits may include less tissue damage, less postoperative pain, and faster recovery for the right patient. That said, not every hospital or surgical center offers the same techniques, and not every patient is a great candidate.
4) Endoscopic Discectomy
Endoscopic discectomy is a newer, highly minimally invasive option in which the surgeon uses a small camera (endoscope) and tiny instruments through a very small incision. Some orthopedic sources note possible benefits such as smaller incisions, less scarring, and shorter recovery time.
It can be a great option in selected cases, but surgeon experience and case selection matter a lot here. “Newer” is not automatically better for every spine.
5) Cervical Procedures (Front-of-Neck Approaches, Fusion, or Disc Replacement)
When the herniated disc is in the neck (cervical spine), the operation may be different from a lumbar microdiscectomy. A common approach is an anterior cervical discectomy and fusion (ACDF), where the surgeon removes the damaged disc from the front of the neck and stabilizes the area with a fusion. In selected patients, an artificial disc replacement may be considered instead of fusion.
This is why two people can both say, “I had herniated disc surgery,” but have very different scars, recovery plans, and instructions.
How the Procedure Usually Works
Every surgeon has a specific protocol, but most herniated disc surgeries follow the same overall flow.
Before Surgery
- Evaluation: Physical exam, symptom review, and imaging (often MRI) to confirm the disc is truly the source of symptoms.
- Medication review: You may be told to stop or adjust blood thinners or certain supplements.
- Fasting: If general anesthesia is planned, you will usually need to avoid food and drink for a set period before surgery.
- Planning: Your surgeon explains the approach, likely benefits, alternatives, and risks.
During Surgery
For a typical lumbar discectomy or microdiscectomy, the surgeon usually:
- Makes a small incision over the affected level (or a larger one for an open approach).
- Uses imaging guidance (such as X-ray/fluoroscopy) to confirm the correct spinal level.
- Moves tissue gently aside (or uses tubular retractors in MIS surgery).
- Removes the herniated disc fragment pressing on the nerve.
- Closes the incision and places a dressing.
In many cases, the surgeon removes only the damaged portion of the disc that is causing nerve compression. If the entire disc must be removed in certain situations, additional stabilization (such as fusion) may be needed.
After Surgery
Many discectomy proceduresespecially minimally invasive onesare outpatient, meaning you go home the same day after monitoring in recovery. Some patients stay longer, particularly if they have other medical issues, had a more extensive procedure, or need extra pain control.
It is normal to receive instructions about:
- Incision care
- When to walk and how much
- Lifting and bending restrictions
- Pain medication use
- When to call the surgeon
- Follow-up visits and possible physical therapy
Risks and Possible Complications
Herniated disc surgery is commonly performed and is often very successful, but no surgery is risk-free. The exact risks depend on the procedure type, the spinal level, your general health, and whether it is a first-time or revision surgery.
General Surgical Risks
- Reaction to anesthesia
- Bleeding
- Infection
- Blood clots
Procedure-Specific Spine Risks
- Nerve injury or irritation
- Cerebrospinal fluid (CSF) leak / dural tear
- Persistent pain or only partial relief
- Recurrent disc herniation (the disc herniates again)
- Need for additional surgery later
Some centers also note that a small number of patients may get short-term relief but need further treatment later. That is not a sign you “failed” recoveryspines are complicated, and long-term outcomes depend on the original injury, nerve compression duration, activity demands, and overall disc health.
Recovery: What to Expect (Without the Sugarcoating)
Recovery is where people want a straight answer, and the honest one is: it varies. But there are common patterns.
First 24–72 Hours
You may feel soreness at the incision site, stiffness, and some fatigue. Many people notice that the sharp leg pain improves quickly, while numbness or tingling may take longer. It is also possible to have a brief flare of pain after surgery before things settle down.
Week 1–2
Walking is usually encouraged early (short, frequent walks). Sitting too long may feel uncomfortable. Many surgeons want patients to avoid repeated bending, twisting, and lifting during this phase. Depending on your surgery and your doctor’s instructions, you may also have limits on driving and work activities.
Some people with desk jobs can return fairly early, while others need more time. If your job involves lifting, climbing, or operating machinery, your timeline is usually longer.
Week 2–6
This is the “doing better, but not invincible” phase. Many people feel much better and start trying to do everything at once. That is usually the part your spine dislikes.
Common recommendations in this window include:
- Gradually increasing walking distance
- Following lifting restrictions carefully
- Using good posture (especially with sitting)
- Starting physical therapy if prescribed
- Returning to activity step by step, not all at once
Some sources note that return to work can happen in about 1–2 weeks for certain minimally invasive cases, while others cite a broader 2–6 week range depending on job demands. Both can be true. A software engineer and a warehouse worker do not get the same recovery schedule.
Longer-Term Recovery
Even when the surgical pain improves fast, the spine still needs time. Nerves can take weeks or months to calm down, especially if they were compressed for a long time before surgery.
Long-term recovery usually focuses on:
- Core and hip strength
- Body mechanics (how you lift, sit, and move)
- Weight management if recommended
- Avoiding repetitive bending/twisting under load
- Consistent movement rather than total rest
The big goal is not just “heal the incision.” It is “reduce the chances of meeting your surgeon again for the same disc.”
When to Call Your Doctor During Recovery
Call your healthcare team promptly if you notice any of the following:
- Fever or chills
- Increasing redness, swelling, or drainage from the incision
- Severe or worsening pain that does not improve with medication
- New weakness or worsening numbness
- Loss of bowel or bladder control
- Severe headache, especially if worse when upright (possible CSF leak in some cases)
Always follow your own surgeon’s discharge instructions first, because they may be tailored to your exact procedure.
FAQ: Quick Answers People Usually Want First
Is herniated disc surgery always a discectomy?
Not always. “Discectomy” is common, especially for lumbar herniations, but the exact surgery can vary by location and severity. Cervical cases may involve ACDF or disc replacement in selected patients.
Will surgery fix back pain completely?
It often helps the nerve-related pain (especially leg pain/sciatica) more than it helps generalized back pain. Many patients improve a lot, but no surgeon can promise a perfect, permanent result.
How long until I feel normal again?
Some people feel dramatically better in days. Others need several weeks to months for nerves to settle down and strength to return. Recovery speed depends on the procedure, your health, and how long the nerve was compressed before surgery.
Can a herniated disc come back after surgery?
Yes, recurrence can happen. That is one reason surgeons emphasize movement habits, physical therapy, and gradual return to activity.
Experiences People Commonly Report After Herniated Disc Surgery (Extended Section)
Real recovery stories are rarely as neat as a discharge handout. Most people expect one of two outcomes: “I wake up totally fixed” or “I’m doomed forever.” In reality, recovery is usually somewhere in the middleand that middle is often very normal.
A common experience is fast relief of the original nerve pain but slower recovery of everything else. For example, someone with severe sciatica might wake up and say, “The lightning bolt down my leg is finally gone,” but then notice incision soreness, stiffness, and fatigue for a week or two. That is not a contradiction; it is actually a pretty typical pattern.
Another common experience is the “good day, bad day” cycle. A patient may feel great on Tuesday, do a little too much on Wednesday (laundry counts, unfortunately), and feel sore on Thursday. People sometimes panic and assume the surgery failed. Usually, the issue is that tissues are healing, nerves are still sensitive, and the body is not ready for a full-speed return yet. Recovery tends to improve in a zigzag, not a straight line.
Desk workers often report a surprising challenge: sitting can feel harder than walking early on. Walking is usually encouraged and often feels better because it keeps the body moving. Sittingespecially with poor posturecan put pressure on healing structures and irritate symptoms. This is why many people build a temporary routine with short walks, position changes, and gentle breaks rather than trying to “power through” a full workday in one chair.
People with physically demanding jobs tend to describe a different challenge: they may feel better before they are truly ready to lift, twist, or carry heavy loads. That gap between “I feel okay” and “my spine is ready” is where setbacks happen. The most successful recoveries are often the least dramatic: steady walking, careful body mechanics, physical therapy when prescribed, and a gradual return to normal activity.
It is also very common for numbness or tingling to improve more slowly than pain. Nerves heal on their own schedule, and they are not in a hurry. Some patients notice strength returning first, others notice pain reduction first, and some have lingering tingling for a while even when the surgery worked well. This can be frustrating, but it does not automatically mean something is wrong.
Emotionally, many patients describe a strange mix of relief and fear. Relief because the worst pain is finally improving; fear because they do not want to re-injure the disc. That fear is understandable. It often gets better once people learn a simple recovery framework: move often, avoid the motions your surgeon restricted, and build confidence with safe activity instead of total rest.
One of the most encouraging experiences people report is the return of “ordinary life” momentsputting on socks without a wrestling match, sleeping through the night, taking a walk without leg pain, or driving without counting every second. Those little wins are easy to overlook, but they are often the clearest signs that recovery is working.
If there is one recovery lesson patients repeat over and over, it is this: listen to your surgeon, and don’t compare your timeline too much to someone else’s. Two people can have the same diagnosis and completely different recoveries because of age, fitness, job demands, nerve compression duration, and surgical technique. Slow progress is still progress.
Final Takeaway
Herniated disc surgery is not the first step for most peoplebut for the right patient, it can be a major turning point. The best results usually come from good timing, clear imaging and symptoms that match, the right surgical approach, and a smart recovery plan that respects the healing process.
If you are considering surgery, ask your surgeon three practical questions: Why this procedure? What is my realistic recovery timeline for my job and lifestyle? and What are the red flags after surgery? Those answers matter just as much as the name of the procedure itself.