Table of Contents >> Show >> Hide
- What is hidradenitis suppurativa (HS)?
- Hidradenitis suppurativa pictures: What HS typically looks like
- Symptoms of hidradenitis suppurativa
- What causes hidradenitis suppurativa?
- How HS is diagnosed
- Treatment for hidradenitis suppurativa
- At-home and lifestyle strategies (the unglamorous heroes)
- Over-the-counter support: What may help
- Prescription topical treatments (often for mild HS)
- Oral medications (when HS is more frequent or widespread)
- Biologics and advanced immune-targeting treatments
- Procedures and surgery (especially for tunnels or persistent areas)
- What a realistic treatment plan can look like (specific examples)
- Complications and related conditions
- When to see a doctor
- Living with HS: Strategies that make day-to-day easier
- Real-Life Experiences and What People Wish They Knew (About )
- Conclusion
If you’ve ever Googled “hidradenitis suppurativa pictures” at 2 a.m. and immediately regretted it (hello, incognito mode),
you’re not alone. Hidradenitis suppurativa (HS)also called acne inversais a chronic inflammatory skin condition that tends to show up
in the exact places you’d rather not discuss in polite conversation: underarms, groin, buttocks, inner thighs, and under the breasts.
It can be painful, frustrating, and wildly misunderstood. The good news? HS is treatable, and many people find a routine and treatment plan
that dramatically reduces flare-ups.
This guide walks through what HS typically looks like (without the nightmare fuel), common symptoms, why it happens, how doctors diagnose it,
and the full menu of treatment optionsfrom at-home strategies to prescription meds to procedures. We’ll keep it real, keep it useful,
and keep it respectful.
What is hidradenitis suppurativa (HS)?
HS is a long-term inflammatory condition that starts around hair follicles in areas where skin rubs together. It’s not caused by being “dirty,”
and it’s not contagious. HS tends to come and go in flare-ups. Over time, repeated inflammation can lead to scarring and “tunnels” under the skin
(often called sinus tracts). That sounds dramatic because it isbut early diagnosis and proper treatment can help prevent HS from progressing.
HS vs. “just boils”
A single boil can happen to anyone. HS is different because it’s usually recurrent, shows up in similar locations,
and may leave scars or persistent lumps. Many people are misdiagnosed for years because HS can resemble folliculitis, infected cysts,
or “stubborn acne.”
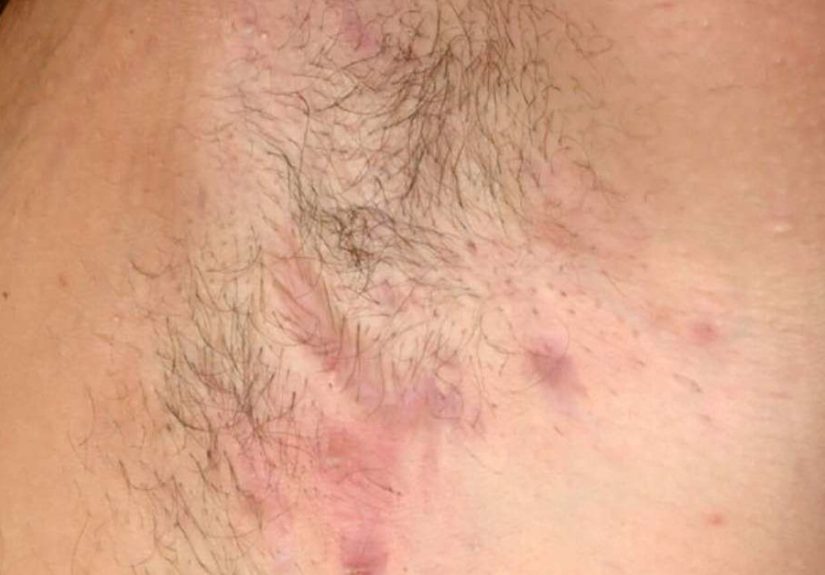
Hidradenitis suppurativa pictures: What HS typically looks like
Let’s talk about “pictures” in a way that actually helps. HS can look different depending on skin tone, body area, and severity.
If you’re comparing yourself to random internet images, remember: online photos often show extreme cases and don’t represent everyone.
Common visual clues (in plain language)
- Tender bumps under the skin that may start small and feel sore or deep.
- Clusters of bumps in friction-prone areas (underarms, groin, inner thighs, buttocks, under breasts).
- Blackheadssometimes appearing in pairs (“double” blackheads) in the same general area.
- Areas that repeatedly flaresame neighborhood, different day.
- Scarring or thickened skin where flares have come and gone.
What HS pictures can’t show
Photos don’t capture the full experience: the pain, the swelling, the way friction or heat can trigger a flare, or the emotional stress.
If you think you might have HS, a dermatologist’s evaluation matters more than a “this looks like that” moment on your phone screen.
A practical tip: Using photos for tracking
Many people find it useful to take private, secure progress photos (only if you feel comfortable) to track flare patterns.
That information can help your clinician see whether a treatment is working, especially if symptoms come and go.
If photos feel too personal, a simple note like “left underarm, same spot, twice this month” works too.
Symptoms of hidradenitis suppurativa
HS symptoms vary from mild to severe. Some people have occasional flare-ups; others deal with frequent, painful inflammation.
Symptoms often begin in the teens or 20s, but HS can appear at other ages too.
Typical symptoms
- Recurring painful lumps under the skin, especially in skin-fold areas.
- Inflammation and swelling that may worsen with friction, heat, or sweating.
- Drainage from affected areas during flares (often the part nobody wants to talk aboutbut it’s common).
- Scarring or thickened skin after repeated flares.
- Skin tunnels (in more advanced HS), which can connect inflamed areas under the skin.
HS severity: The Hurley stages (a common framework)
Clinicians often describe HS using the Hurley staging system:
- Hurley Stage I: Isolated or occasional lumps/abscess-like lesions, without tunnels or extensive scarring.
- Hurley Stage II: Recurrent lesions with some scarring and limited tunnels; flare areas may be more spread out.
- Hurley Stage III: More widespread involvement with multiple connected tunnels and significant scarring.
What causes hidradenitis suppurativa?
HS isn’t a hygiene problem, and it’s not “because you shaved wrong once.” HS is driven by inflammation around hair follicles,
and genetics can play a role. Many researchers describe HS as an autoinflammatory conditionmeaning the immune system is overly reactive in certain skin areas.
Common risk factors and triggers
- Family history: HS can run in families.
- Smoking: Strongly associated with HS and worse flare patterns in many people.
- Excess weight: Not a “blame” issuemore friction and inflammation can worsen symptoms.
- Friction and sweating: Tight clothing, rubbing, and heat can trigger flare-ups.
- Hormonal factors: Some people notice flares around menstrual cycles.
Is hidradenitis suppurativa contagious?
No. HS is not contagious. You can’t “catch” it from someone, and you can’t give it to someone else by sharing towels.
(That said, if skin is draining, basic hygiene and wound care are still important to reduce the chance of secondary infection.)
How HS is diagnosed
HS is usually diagnosed clinicallymeaning a clinician recognizes patterns: recurring lesions, typical locations, and scarring/tunnels over time.
There isn’t a single definitive lab test that “proves” HS.
What your dermatologist may ask
- Where do flares occur (underarms, groin, etc.)?
- How often do they come back, and do they reappear in the same spots?
- Any family history?
- Any triggersheat, friction, menstrual cycle, stress, smoking?
- What treatments have you tried (and what made it worse)?
Conditions that can mimic HS
HS can resemble folliculitis, boils, infected cysts, acne, and other inflammatory or infectious skin problems.
This is one reason HS is sometimes diagnosed lateespecially when symptoms are mild early on.
Treatment for hidradenitis suppurativa
HS treatment is usually a mix of strategies: reducing inflammation, managing flare-ups early, preventing new lesions,
and treating tunnels/scarring when needed. The right plan depends on severity, affected areas, and your health history.
Many people need a “combo approach,” and it often takes some trial-and-adjust to find what truly works.
At-home and lifestyle strategies (the unglamorous heroes)
- Reduce friction: Choose loose, breathable clothing; avoid seams that rub flare-prone areas.
- Gentle cleansing: Mild, fragrance-free cleansers can help; harsh scrubs usually backfire.
- Warm compresses: Can soothe discomfort and encourage drainage naturally (no squeezing).
- Hair removal caution: If shaving triggers flares, consider alternatives; laser hair reduction may help some people.
- Smoking cessation: Quitting can reduce flare frequency and severity for many.
- Weight management (if relevant): Even modest changes can reduce friction and inflammation in some people.
The goal isn’t “be perfect.” It’s to lower the everyday triggers that keep HS simmering. Think of it like turning down the heat under a pot
so it stops boiling over.
Over-the-counter support: What may help
Some people use OTC benzoyl peroxide washes or antiseptic washes as part of their routine, especially if they’re prone to secondary irritation.
These aren’t cures, and they can be dryingso they’re best used thoughtfully and ideally with clinician guidance.
Prescription topical treatments (often for mild HS)
- Topical antibiotics: Clindamycin is commonly used for mild HS or localized flares.
- Topical resorcinol: In some cases, clinicians recommend it to help with follicular plugging and discomfort.
- Intralesional steroids: A clinician can inject a steroid into an inflamed lesion to reduce pain and swelling faster.
Oral medications (when HS is more frequent or widespread)
- Oral antibiotics: Tetracyclines (like doxycycline) are often used for their anti-inflammatory effects.
Some regimens use combination antibiotics (for example, clindamycin with rifampin) for more persistent disease. - Hormonal approaches: For some women, certain oral contraceptives or spironolactone may help if flares are hormonally influenced.
- Metformin (selected cases): Sometimes used when insulin resistance or PCOS is part of the picture.
- Pain control: Anti-inflammatory medications or other pain strategies may be recommendedbecause “just ignore it” is not a plan.
Biologics and advanced immune-targeting treatments
For moderate-to-severe HS, biologic medications can be game-changing. These are prescription therapies that target specific immune pathways driving inflammation.
As of recent FDA approvals, biologics specifically approved for HS include:
- Adalimumab (approved for moderate-to-severe HS, including certain patients ages 12+).
- Secukinumab (approved for adults with moderate-to-severe HS).
- Bimekizumab (approved for adults with moderate-to-severe HS).
Biologics aren’t for everyone, and they require medical oversight. But if HS is affecting your life, school, work, mobility,
sleep, or mental health, it’s worth asking a dermatologist whether you’re a candidatebecause “white-knuckling it” shouldn’t be the long-term strategy.
Procedures and surgery (especially for tunnels or persistent areas)
When HS forms tunnels or repeatedly flares in the same spot, procedures can provide more lasting relief than repeated short-term fixes.
Options may include:
- Deroofing (unroofing): A procedure that opens and removes the “roof” over tunnels so the area can heal more effectively.
- Excision: Surgical removal of chronically affected tissue in a localized area.
- Laser approaches: Some lasers reduce hair follicles and inflammation; others can target damaged tissue in select cases.
- Drainage procedures: Sometimes used for immediate relief, but they may not prevent recurrence if HS is ongoing.
What a realistic treatment plan can look like (specific examples)
HS care works best when it’s tailored. Here are examples of how treatment often escalatesjust to show what “normal” can look like:
Example 1: Mild, occasional HS (Hurley I)
- Daily friction reduction (looser clothing, moisture control)
- Gentle cleansing routine; consider clinician-recommended antibacterial wash
- Topical clindamycin during flares
- Early intervention: warm compresses, no squeezing, quick check-ins if flares increase
Example 2: Moderate HS with frequent flares (Hurley I–II)
- Topical plus oral anti-inflammatory antibiotic course (often several weeks to months)
- Trigger review (smoking, friction, weight changes, menstrual cycle patterns)
- Consider hormonal therapy (when appropriate)
- Discuss laser hair reduction for recurrent areas
- Mental health screening and support (HS has a real quality-of-life impact)
Example 3: More advanced HS with tunnels (Hurley II–III)
- Biologic therapy consideration (and sometimes combination therapy)
- Targeted procedures like deroofing for persistent tunnels
- Wound-care strategy that fits daily life (supplies, clothing, routines)
- Coordination with other specialists if comorbidities are present (for example, metabolic issues or inflammatory conditions)
Complications and related conditions
HS isn’t only a skin issue. Chronic inflammation and pain can affect sleep, movement, social life, and mental health.
HS is also associated with a higher likelihood of certain comorbidities, including depression/anxiety and metabolic issues.
If HS is affecting how you feel emotionally, that counts as a medical issuenot “being dramatic.”
When to see a doctor
Consider medical evaluation if you have recurring painful lumps in typical HS areas, especially if they return in the same spots,
leave scars, or interfere with walking, sitting, sleep, sports, or daily life. Seek prompt care if you develop fever, rapidly worsening swelling,
or feel generally unwell during a flare.
Living with HS: Strategies that make day-to-day easier
- Build a flare plan: Know what you’ll do at the first warning signcompress, topical medication, reduce friction, contact your clinic if needed.
- Choose “HS-friendly” clothes: Soft seams, breathable fabric, less rubbing. Comfort isn’t laziness; it’s prevention.
- Make movement workable: If exercise helps your mood but friction triggers flares, try lower-friction options (cycling shorts under loose layers, moisture-wicking fabrics, shorter sessions).
- Don’t self-blame: HS is not a moral failing. It’s an inflammatory condition that deserves treatment.
Real-Life Experiences and What People Wish They Knew (About )
HS doesn’t just show up on the skinit shows up in calendars, closets, confidence, and the “do I really have to go today?” moments.
A lot of people describe the early HS experience as confusing: a tender bump appears, it goes away, then it comes back like it pays rent.
Because HS often affects private areas, many people delay getting care. They might assume it’s an ingrown hair, a random boil,
or something they “caused.” That delay is incredibly commonand it’s also why a diagnosis can feel like both relief and rage:
relief that there’s a name for it, and rage that it took so long to get that name.
Many people say the most helpful shift was reframing HS from “something I need to hide” into “a condition I can manage.”
That doesn’t mean you have to become a full-time HS influencer with matching motivational quotes. It means building small,
realistic habits that reduce flares. For example: switching from tight seams to softer, breathable fabrics can cut down friction.
Keeping a simple “flare kit” (clean gauze, gentle tape, fragrance-free wipes, whatever your clinician recommends) can reduce panic when a flare starts.
And learning your triggersheat, sweat, certain shaving routines, stress spikescan help you make better choices without feeling like your life is shrinking.
There’s also the emotional side. HS can make people feel isolated because it’s not exactly dinner-table conversation.
Some people avoid the gym, sports, dating, or even raising their hand at school because they’re worried about discomfort or visible marks.
What often helps is having at least one safe persona friend, parent, partner, school nurse, or clinicianwho understands that HS pain is real.
People also frequently mention how validating it feels when a dermatologist takes HS seriously and offers a plan instead of a shrug.
If your first provider doesn’t get it, that doesn’t mean you’re out of options; it means you need someone who treats HS often.
Treatment journeys can be a bit like trying on shoes: the first pair might not fit, and you’re allowed to change them.
Mild HS might improve with topical medication and lifestyle tweaks. Moderate disease may need oral medications and procedural options.
More severe HS may respond best to biologics and targeted surgical approaches. What many people wish they’d known sooner is that needing escalation
doesn’t mean you “failed.” It means HS is an inflammatory condition that sometimes requires stronger tools.
Finally, there’s a practical truth most people learn the hard way: squeezing, picking, and aggressive scrubbing almost never help.
HS thrives on irritation. Gentler care and earlier treatment tend to win. And if you’re feeling overwhelmed, you’re not weakyou’re human.
HS can be a lot. But with a smart plan, supportive care, and the right clinician team, many people go from “constant flare anxiety”
to “I have flare-ups sometimes, and I know what to do.”
Conclusion
Hidradenitis suppurativa can be painful and emotionally exhausting, but it’s not hopelessand it’s not your fault.
Understanding what HS looks like, recognizing symptoms early, and working with a dermatologist on a step-by-step treatment plan
can dramatically improve quality of life. Whether you’re dealing with mild flare-ups or more advanced disease,
today’s HS treatments include effective topicals, oral medications, biologics, and procedures that can reduce recurrence and help prevent progression.
The most important step is getting the right diagnosis and building a plan that fits your real life.