Table of Contents >> Show >> Hide
Heart rate variability, or HRV, has become the darling of smartwatches, fitness rings, recovery apps, and the kind of people who know exactly how many minutes they spent in REM sleep. It sounds technical, slightly mysterious, and just serious enough to make you wonder whether your body is thriving or quietly filing complaints.
So how relevant is heart rate variability, really? Quite relevant, actually, but not in the dramatic, crystal-ball way social media sometimes suggests. HRV can be a useful window into stress, recovery, sleep quality, fitness, and overall resilience. But it is not a one-number verdict on your health, and it is definitely not a replacement for symptoms, medical history, or a real conversation with a clinician.
The smartest way to think about HRV is this: it is a context clue, not a courtroom sentence. When used well, it can help you understand how your body is adapting to life’s demands. When used badly, it can turn a perfectly nice morning into a panic spiral because your wrist gadget decided you were “strained.” Your watch may be clever, but it still doesn’t know you stayed up late helping your cousin move furniture and then ate spicy noodles at 11:30 p.m.
What heart rate variability actually means
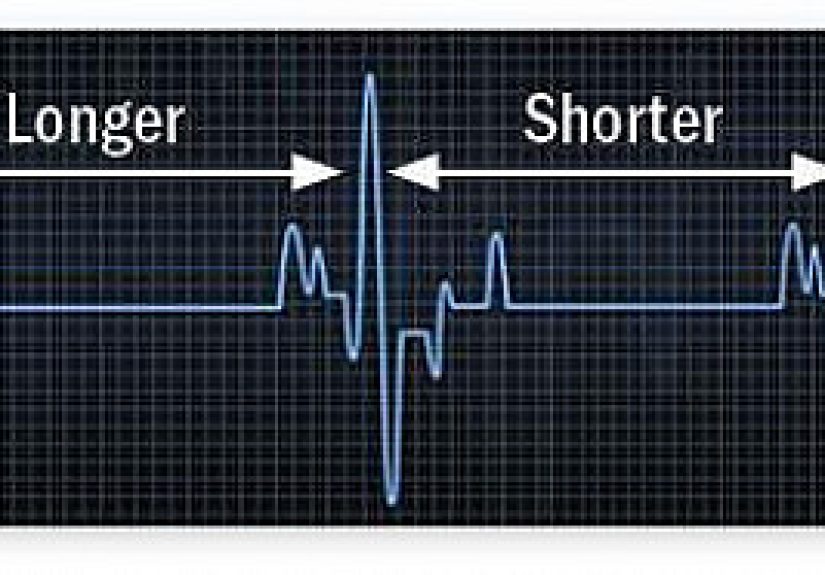
HRV measures the tiny differences in time between one heartbeat and the next. Even if your heart is beating 60 times per minute, those beats are not spaced like perfect metronome clicks. The interval changes slightly from beat to beat, often by milliseconds. That variability is normal. In fact, some variability is a sign that the body is adjusting well to internal and external demands.
This matters because HRV reflects activity in the autonomic nervous system, the system that manages automatic functions such as heart rate, breathing, blood pressure, and digestion. One branch leans toward action and alertness, often called the “fight-or-flight” response. The other supports rest, recovery, and restoration. HRV gives a rough sense of how flexible that system is. A higher HRV often suggests the body is adapting efficiently. A lower HRV may suggest strain, fatigue, illness, poor recovery, or other stressors.
That does not mean high is always heroic and low is always disastrous. HRV is highly individualized. Age, genetics, fitness, hormones, medications, sleep, alcohol, emotional stress, underlying medical conditions, and even the device being used can all influence the number. One person’s “great” score may be another person’s Tuesday.
Why a variable heartbeat can be a good thing
People often assume a healthy heart should beat with machine-like regularity. That sounds logical, but biology loves nuance. A heart that can speed up, slow down, and subtly adjust beat-to-beat timing in response to breathing, recovery, and daily demands is showing adaptability. In many cases, that flexibility is what you want.
Think of HRV as a sign of responsiveness. A resilient body is not rigid. It adjusts. It recalibrates. It handles a difficult workout, a bad night of sleep, a stressful meeting, or a long travel day without acting like the world just ended. That is where HRV becomes relevant.
Why HRV matters in everyday health
The real value of HRV is not that it tells you something brand-new about human biology. It is that it can make invisible stress more visible. Sleep loss, emotional strain, dehydration, illness, and intense training can all nudge HRV downward. Good recovery habits can help move it in a healthier direction over time.
For active people, HRV can be useful as a recovery signal. If your baseline is usually steady and then drops for several days while your resting heart rate climbs, your sleep gets worse, and you feel sluggish, that may be your body asking for a lighter training day. Not in a diva way. More in a “please stop treating me like a rental car” way.
For people focused on stress management, HRV can act like a feedback loop. Meditation, breathing exercises, better sleep habits, regular movement, and less alcohol often improve recovery patterns. The benefit is not just the number itself. The benefit is that the number may reinforce healthier choices you were already supposed to be making anyway.
HRV also has a broader medical relevance. Lower HRV has been associated in research with poorer autonomic balance and, in some settings, worse cardiovascular outcomes. That is one reason HRV has been studied in cardiology, aging, sleep research, and stress physiology. Still, the presence of an association does not mean your daily app score should be interpreted like a lab test result.
Sleep, stress, and HRV are constantly negotiating
One of the clearest reasons HRV is relevant is that it often tracks with sleep and stress. Poor sleep can push HRV down. Chronic stress can do the same. That makes sense physiologically: when the body stays revved up, it tends to show less flexibility in autonomic regulation.
This is why overnight HRV measurements are often more useful than random daytime snapshots. During sleep, there is less noise from walking, coffee, meetings, traffic, workouts, and surprise existential dread. Overnight readings usually offer a cleaner look at recovery status, which is why many wearables focus on nighttime data.
Where HRV gets overhyped
Now for the reality check. HRV is relevant, but it is not magic. Consumer wellness culture sometimes treats it like a universal score for health, performance, mood, and destiny. That is where the trouble starts.
First, there is no single “normal” HRV value that applies to everyone. Unlike basic blood pressure categories or resting pulse ranges, HRV does not come with one neat gold-star cutoff. Different devices use different methods and metrics. Your age matters. Your body matters. Your baseline matters more than someone else’s screenshot.
Second, device accuracy varies. Medical-grade electrocardiogram measurements remain the most reliable standard. Chest straps and carefully controlled measurements can be quite useful. Wrist-based optical sensors are convenient, but they are more vulnerable to motion, signal noise, and algorithmic guesswork. Convenience is great. Convenience is not the same as clinical certainty.
Third, HRV is not an arrhythmia detector, not a diagnostic verdict, and not a substitute for symptoms. If you have chest pain, fainting, significant shortness of breath, or persistent palpitations, you need medical evaluation. A reassuring app trend should not talk you out of common sense. Neither should a dramatic app alert convince you that you have a cardiac emergency when you really just had two espressos, bad sleep, and a stressful commute.
One low score should not ruin your day
This may be the most practical point of all. HRV is most useful as a trend, not a headline. A single bad reading can happen for all sorts of boring reasons: poor sleep, alcohol, dehydration, late meals, travel, mental stress, illness, or a hard workout. Boring reasons are still real reasons.
So if your HRV dips one morning, do not immediately assume your body is collapsing like a dramatic soap opera character. Look for patterns. Has it been falling for several days? Do you also feel worse? Is your resting heart rate up? Are you fighting a cold? Did you sleep badly all week? HRV becomes meaningful when it is read in context.
How to use HRV without becoming obsessed
The best approach is to use HRV as a personal trend line. Compare you to you. Track it over weeks, not emotionally over breakfast. If you notice that your HRV tends to be better when you sleep seven to nine hours, train sensibly, hydrate well, and avoid alcohol at night, that is useful information. If it tanks after three straight days of stress and short sleep, that is also useful. The goal is not to chase a perfect score. The goal is to learn how your body responds.
Pair HRV with other signals. Resting heart rate, sleep quality, energy level, mood, soreness, performance, and symptoms all matter. A lower-than-usual HRV with a normal mood, decent sleep, and good energy may not mean much. A lower-than-usual HRV with rising resting heart rate, fatigue, irritability, and a scratchy throat is a different story.
It also helps to think experimentally. Instead of asking, “Is my HRV good?” ask, “What seems to improve or worsen my recovery?” Earlier dinners, consistent bedtimes, reduced alcohol, stress management, and smarter exercise programming often make a bigger difference than people expect. HRV can serve as feedback for those habits, not as a personality test administered by your watch.
Can you improve HRV?
Often, yes, at least over time. Regular exercise tends to help. So do better sleep habits, stress reduction practices, good hydration, a heart-healthy diet, and limiting alcohol. Slow breathing and mindfulness practices may support relaxation and recovery. Treating underlying issues such as sleep problems, anxiety, uncontrolled blood pressure, or other medical conditions may help as well.
But the point is not to “hack” HRV like it is a video game bonus level. The number usually improves when the underlying habits improve. If your goal becomes squeezing out one more millisecond while ignoring your actual quality of life, the wellness app has won and you have lost.
When HRV becomes medically important
HRV has real scientific and clinical relevance, especially in research and formal monitoring. It has been studied as a marker of autonomic function, recovery, stress burden, sleep quality, aging, and cardiovascular risk. In medical settings, clinicians may use ECG-based tools or longer monitoring such as Holter monitors when rhythm issues or symptoms need evaluation.
Still, for the average healthy adult using a wearable, HRV is best viewed as a wellness metric with useful clues, not as a stand-alone medical test. It may help prompt better choices or a more informed discussion with a doctor. It should not be asked to do more than it can reliably do.
And yes, there is exciting research suggesting wearable-measured HRV shifts may help detect changes in health status, including oncoming illness, before people feel obviously sick. That is promising. It is also still evolving. “Interesting” is not the same as “clinically settled.”
Common experiences with HRV in real life
One reason HRV has become so popular is that people often notice it reacting before their daily routine catches up. A runner may see a sudden dip after a week of hard training and shrug it off at first. Then the puzzle pieces line up: legs feel heavy, motivation drops, sleep gets choppy, and the usual workout feels strangely expensive. In that situation, HRV is not predicting the future like a superhero gadget. It is simply reflecting the body’s reduced recovery capacity. The useful move is not panic. It is adjustment. Easier training, more sleep, and a bit less ego often work better than forcing another “grind” session.
Another common experience happens with stress. Someone with a demanding job may notice that their HRV falls during busy stretches, especially when meals get irregular, bedtime gets later, and every email feels like it was written by a small tornado. Then a calmer week arrives, they walk more, breathe a little deeper, sleep better, and the number begins to rebound. In that case, HRV becomes valuable because it turns abstract stress into something visible. It can validate what the body has been trying to say all along: stress is not just “in your head.” It shows up in recovery, mood, patience, and physical resilience.
Parents often describe another pattern. Life gets loud, sleep gets chopped into weird fragments, and recovery becomes a luxury item. HRV may stay lower than expected during those seasons, even if overall health is still good. That does not mean something is necessarily wrong. It often means context matters. A lower baseline during a sleep-deprived phase of life may be less about disease and more about the simple fact that humans do not recover brilliantly when they are awakened at 2:17 a.m. by a child who urgently needs to discuss a stuffed animal emergency.
Then there is the classic “I think I’m getting sick” experience. Some people notice their HRV drops sharply for a day or two before they develop obvious symptoms. They may feel only slightly off at first, maybe a little flat, maybe oddly tired. Later, a cold, virus, or other illness becomes more obvious. This is one reason HRV fascinates both researchers and consumers. It seems to catch the body in transition. Still, this is where restraint matters. A lower HRV can happen for many reasons, so it should invite awareness, not self-diagnosis.
Older adults sometimes have a different experience with HRV. They may discover that their number is lower than a younger relative’s and assume that means they are in poor shape. Not necessarily. HRV tends to decline with age, so comparisons across generations are mostly a waste of perfectly good emotional energy. What matters more is the individual pattern, overall cardiovascular health, symptoms, physical function, and how the number behaves over time.
Perhaps the most important real-life experience is learning not to obsess. Many people start tracking HRV with curiosity and end up checking it too often, assigning meaning to every wiggle in the graph. The healthier long-term experience is usually the opposite: you learn your baseline, you notice your patterns, and then you stop giving every single morning score the power to narrate your entire day. That is when HRV becomes genuinely useful. It becomes feedback, not fear.
Final verdict: relevant, but only if you use it wisely
So, how relevant is heart rate variability? Relevant enough to take seriously, but not so powerful that it deserves its own throne. HRV is most useful as a personalized marker of recovery, resilience, and autonomic balance. It can help connect sleep, stress, exercise, and lifestyle habits to how your body is actually functioning. That is valuable.
At the same time, HRV should be handled with humility. It is influenced by many factors, it varies from person to person, and consumer wearables are not perfect measuring tools. The best use of HRV is to track trends, learn your own baseline, and combine the data with common sense, symptoms, and medical advice when needed.
In other words, HRV matters. Just do not turn it into a tiny digital dictator. Let it be what it is: a helpful clue from your nervous system, not the final word on your health.





