Table of Contents >> Show >> Hide
Measles has an irritating habit of showing up right when people start treating it like a dusty chapter from an old history book. For years, many Americans thought of measles as something their grandparents worried about, somewhere between polio and rotary phones. But recent outbreaks have shattered that illusion. Measles is not a nostalgic disease. It is a highly contagious virus that takes advantage of every crack in the public health wall, and when those cracks widen, it does not politely wait its turn.
That is why the real question is not simply why measles is back in headlines. The better question is why outbreaks keep finding room to grow in a country that has a safe and highly effective vaccine. The answer is uncomfortable, because the root of the problem is not one thing. It is a tangled mix of declining vaccination coverage, misinformation, access barriers, delayed routine care, global travel, and the dangerous clustering of under-vaccinated communities. In other words, measles is not just exposing weak immune systems. It is exposing weak spots in trust, policy, and prevention.
Why measles spreads so fast
Measles is often described as one of the most contagious infectious diseases on Earth, and that is not public health drama for the sake of drama. It spreads through the air when an infected person coughs, sneezes, or even just breathes in a shared indoor space. The virus can linger in the air and on surfaces for a period after that person has left, which means measles can turn a waiting room, classroom, airport gate, or church nursery into an accidental relay race.
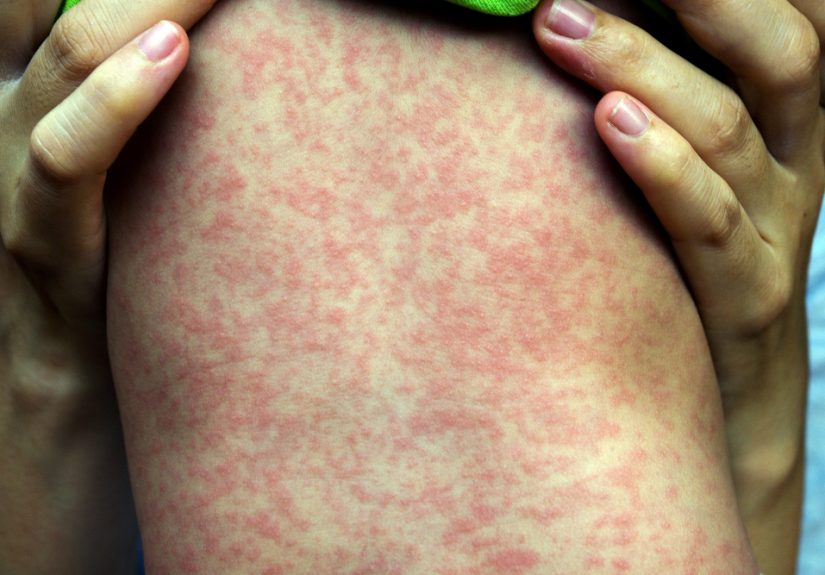
Symptoms usually begin with fever, cough, runny nose, and red watery eyes before the famous rash appears. That detail matters. People can spread measles before the rash makes everyone go, “Well, that seems less than ideal.” By the time the spots appear, exposure has often already happened. This makes measles especially difficult to control once it enters a community with enough unprotected people.
And measles is not just a rash-and-rest illness. It can cause ear infections, diarrhea, pneumonia, dehydration, brain inflammation, and in some cases death. Young children, pregnant people, and individuals with weakened immune systems are at higher risk for severe disease. Even when a patient recovers, measles can leave behind a nasty biological souvenir: a period of immune suppression sometimes described as “immune amnesia,” in which the virus damages existing immune memory and increases vulnerability to other infections later on.
The vaccine works. The gaps are the problem.
The single biggest reason measles outbreaks happen is simple: not enough people are vaccinated in the right places at the right levels. The measles, mumps, and rubella vaccine, or MMR, is remarkably effective. Two doses provide strong protection, and widespread vaccination is what allowed the United States to declare measles eliminated back in 2000. That did not mean the virus disappeared from the planet. It meant continuous local spread had been interrupted.
But elimination is not eradication. Measles still circulates globally, and imported cases can reignite outbreaks when they land in communities with low vaccination coverage. This is why public health experts keep stressing a point that sounds repetitive only because it is so important: measles does not need a giant nationwide drop in vaccination to make a comeback. It needs clusters. A neighborhood, school, county, or social network with lower-than-expected vaccine uptake can be enough to create a foothold.
That is where the root problem gets tricky. A state might report a respectable overall vaccination rate, yet still contain pockets where coverage is far too low to stop spread. Measles does not care that averages look decent on a spreadsheet. It cares whether the people sharing air in a real community are protected.
Getting to the real roots of modern outbreaks
1. Vaccine hesitancy and misinformation
This is the root that gets the most attention, and for good reason. False claims about vaccine safety continue to circulate online, in chat groups, and sometimes even in person from people who speak with the confidence of a surgeon and the evidence base of a potato. Some parents are not fully anti-vaccine, but they are anxious, overwhelmed, or persuaded to “wait a little longer.” In measles prevention, that delay matters.
Experts often describe hesitancy through the “3 Cs”: confidence, complacency, and convenience. Confidence means whether people trust the vaccine, the health system, and the recommendations. Complacency means whether they think measles is still a real threat. Convenience means whether getting vaccinated is easy, affordable, and practical. Outbreaks often grow where all three problems collide.
2. Missed routine care after the pandemic
Routine childhood immunization schedules took a hit during and after the COVID-19 pandemic. Some families postponed wellness visits. Some moved, changed insurance, or lost connection with primary care. Others simply fell out of the habit of preventive medicine. Those missed doses did not stay trapped in the past. They created a larger pool of susceptible children and adolescents in the present.
Even a modest decline in MMR coverage can have an outsized effect because measles is so contagious. Once coverage slips below the level needed for community protection in enough places, outbreaks become easier to start and harder to contain.
3. Access barriers that are less dramatic but very real
Not every undervaccinated child has parents who distrust vaccines. Some families face practical obstacles: limited clinic hours, transportation problems, long waits for appointments, language barriers, paperwork issues, lack of paid leave, or confusion about where to go. Public health failures are often blamed on ideology when logistics also deserve a starring role.
In underserved communities, prevention can lose out to immediate survival priorities. When a parent is choosing between hourly wages, child care, and a doctor’s appointment, the vaccine may be delayed not because it seems unimportant, but because everything else is on fire.
4. Travel and importation
Measles anywhere can become measles here. International travel helps connect families, businesses, and tourism. It also gives infectious diseases frequent-flyer privileges. A traveler exposed abroad can return to the United States before symptoms are obvious, and if that person enters a community with low vaccination coverage, the outbreak chain can begin. Domestic travel then helps the virus keep moving. In a country with busy airports, theme parks, sporting events, and shared indoor spaces, measles does not need a handwritten invitation.
5. Weak public health capacity and delayed response
When measles is suspected, speed matters. Cases need rapid diagnosis, isolation guidance, contact tracing, exposure notifications, school coordination, and vaccination outreach. That work is labor-intensive. It depends on a strong local public health workforce, functioning communication systems, and public cooperation. If staffing is thin or trust is low, the response slows down. Measles loves delay.
Recent outbreaks have shown how disruptive measles can be for health care practices too. Clinics may need special triage procedures to avoid exposing other patients. Schools and child care programs may exclude unvaccinated students during outbreaks. Hospitals must manage infection-control demands that consume time, money, and staff attention. Measles is not just a medical issue. It is an operational headache with a very expensive personality.
Why the issue feels bigger now
Part of the reason measles outbreaks feel more alarming is that they symbolize something larger. They are a warning light on the dashboard of public health. A rise in measles suggests weakening vaccination coverage, fraying trust, and communities that may also be vulnerable to other vaccine-preventable diseases.
By late March 2026, the United States had already recorded a striking number of confirmed measles cases, with multiple jurisdictions reporting spread. That matters not only because of the immediate illnesses, hospitalizations, and deaths linked to outbreaks, but also because it raises concern about whether the country can hold onto the elimination status it achieved years ago. Once that status is threatened, measles stops looking like a local flare-up and starts looking like a structural national problem.
What families and communities can do right now
Check vaccination status early, not during panic mode
The worst time to discover a vaccine gap is after an exposure notice lands in your inbox. Families should review records before travel, school entry, or outbreak season. Children typically receive the first MMR dose at 12 to 15 months and the second at 4 to 6 years. In outbreak settings or for international travel, earlier or additional doses may be recommended for some children, including infants 6 through 11 months in certain circumstances. Adults without evidence of immunity should also talk with a clinician about whether they need vaccination.
Use trusted medical sources, not viral chaos
When measles hits the news, misinformation often arrives wearing running shoes. Parents should rely on pediatricians, state health departments, and major medical organizations rather than social posts, random influencers, or that one cousin who believes vitamins can solve nearly every known problem except bad Wi-Fi. Evidence-based information is not always flashy, but it tends to age better.
Make access easier, not harder
Communities get better outcomes when vaccination is simple. That means school-based clinics, reminder systems, walk-in options, extended hours, multilingual outreach, transportation support, and partnerships with trusted local leaders. Public health wins more often when it is convenient, visible, and respectful.
Respond fast when outbreaks appear
Suspected measles should trigger quick action, not wishful thinking. Parents of symptomatic children should call ahead before visiting a clinic so staff can reduce exposure risk to others. Schools and child care programs need clear outbreak policies. Public messaging should be direct, calm, and practical. Delay gives measles room. Speed takes it away.
The deeper lesson
If measles outbreaks teach one lesson, it is this: success in public health is easy to undervalue because it often looks like nothing happening. No outbreak. No school closure. No child in the hospital with pneumonia from a preventable virus. Prevention is quiet, and quiet is easy to take for granted. Until it is gone.
Getting to the root of the measles problem means being honest about what outbreaks really reveal. They reveal distrust that has not been repaired, systems that are not equally accessible, communities that are more connected by travel than by preventive care, and a culture that sometimes confuses loud opinions with informed judgment. The measles virus is ruthless, but it is also predictable. It goes where protection is weak.
The good news is that the solution is not mysterious. Strong vaccination coverage, quick public health response, clear communication, and easier access to routine care still work. Measles is not unbeatable. But it is very good at punishing complacency. If the United States wants fewer outbreaks, it does not need magic. It needs consistency, trust, and the will to do boring, effective things before a crisis makes them urgent.
Experiences from homes, schools, clinics, and communities
One of the most revealing parts of any measles outbreak is how ordinary the first moments often seem. A child develops a fever and cough. A parent assumes it is a routine virus. A school attendance clerk notices a few more absences than usual. A pediatric office gets a nervous phone call from someone who just learned about a possible exposure at an airport or church event. Nobody begins the week thinking, “Ah yes, this is how public health stress enters the group chat.” But that is often how it starts.
For parents, the experience tends to split into two very different stories. Families whose children are fully vaccinated usually still feel anxious, but their worry comes with a layer of protection and clarity. They call the pediatrician, confirm records, and keep watch. Families with delayed or missing vaccines often experience the outbreak very differently. Suddenly, a decision that once felt abstract becomes immediate. There may be school exclusion rules, urgent appointments, canceled plans, and the awful realization that measles is not just a headline about “other people.” It is now a scheduling problem, a health concern, and an emotional burden inside the home.
Schools and child care programs experience outbreaks as a balancing act between education and infection control. Administrators must answer parent questions, coordinate with health departments, review immunization documentation, and explain why some students may need to stay home. Teachers may worry about vulnerable students, pregnant staff members, or younger siblings at home. Even when a school avoids a large outbreak, the atmosphere can shift quickly from normal routine to low-grade alarm.
Health care workers describe another layer of disruption. Front desk staff may have to screen patients before they enter. Pediatricians may guide families by phone first so a potentially contagious child does not sit next to newborns in a waiting room. Infection prevention teams, already busy, must move even faster. A single suspected case can trigger a long chain of logistics, from room cleaning to exposure notices. In that sense, measles creates ripple effects far beyond the infected person.
Then there are the people whose experiences rarely make the loudest headlines: immunocompromised adults, infants too young for routine vaccination, pregnant people, and families caring for children with serious medical conditions. For them, outbreaks can shrink daily life. Errands become risk calculations. Social gatherings feel less casual. A trip to a clinic or grocery store may require more caution than most neighbors realize. Their experience is a reminder that vaccination is not only an individual choice. It is also a community safety net.
Across all these experiences, the same lesson keeps surfacing. Measles outbreaks are not only about virology. They are about trust, timing, and whether communities make prevention easy before fear takes over. When protection is strong, outbreaks struggle to spread. When it weakens, everyday life gets more complicated for everyone, including people who never expected measles to return at all.
Conclusion
Measles outbreaks do not happen because the virus suddenly got clever. They happen because communities give it openings. The root of the problem is not a mystery, and that is exactly why the issue deserves serious attention. Vaccination gaps, misinformation, delayed routine care, access barriers, and sluggish response systems all make outbreaks more likely. The solution is not glamorous, but it is proven: restore confidence, expand access, strengthen public health response, and keep vaccination coverage high enough that measles has nowhere to go. When prevention works, it looks quiet. That quiet is worth protecting.