Table of Contents >> Show >> Hide
- What Is a Pulmonary Function Test?
- Why Would You Need a Pulmonary Function Test?
- How to Prepare for a Pulmonary Function Test
- What Happens During the Procedure?
- How Long Does a Pulmonary Function Test Take?
- What Do the Results Show?
- Is a Pulmonary Function Test Painful?
- Risks and Safety Concerns
- Who Performs Pulmonary Function Tests?
- Tips for Getting the Most Accurate Results
- Experiences Related to Pulmonary Function Testing
- Conclusion
- SEO Tags
If your doctor orders a pulmonary function test, do not panic. You are not being recruited for astronaut training, and you are not about to be sealed into a giant science-fiction pod forever. A pulmonary function test, often called a PFT, is simply a group of breathing tests that show how well your lungs are working. These tests help measure how much air your lungs can hold, how quickly you can move air in and out, and how effectively oxygen passes from your lungs into your bloodstream.
In plain English, a pulmonary function test helps answer a very important question: Are your lungs doing their job well enough? That matters if you have shortness of breath, a stubborn cough, wheezing, chest tightness, or a lung condition such as asthma, COPD, or pulmonary fibrosis. It also matters before some surgeries, after exposure to smoke or workplace irritants, and when your doctor wants to see whether treatment is helping.
This guide walks through the real purpose of pulmonary function testing, what the procedure is actually like, what the results can reveal, and the risks you should know about before you sit down, put on the nose clip, and blow like you are trying to launch a paper airplane into the next zip code.
What Is a Pulmonary Function Test?
A pulmonary function test is not just one test. It is a category of noninvasive lung tests that measure airflow, lung volume, and gas exchange. Some tests are done at rest, while others may be repeated after you use a bronchodilator or, in some cases, while you exercise.
The most common types include:
1. Spirometry
This is the classic breathing test. You take a deep breath in and then blow out as hard and fast as possible into a mouthpiece connected to a machine called a spirometer. Spirometry helps measure how much air you can exhale and how quickly you can do it. It is often the first test ordered when a provider suspects asthma, COPD, or another condition that affects airflow.
2. Lung Volume Testing or Body Plethysmography
This test measures how much air your lungs can hold and how much air stays trapped inside after you exhale. You usually sit in a clear booth that looks a little like a phone booth’s more medically anxious cousin. It may feel odd for a moment, but it helps providers understand whether your lungs are overinflated, restricted, or somewhere in between.
3. Diffusing Capacity Test
This test checks how well gases move from your lungs into your blood. You breathe in a tiny, safe amount of test gas, often including a trace level of carbon monoxide, hold your breath briefly, and then exhale. The result gives your provider a sense of how efficiently your lungs transfer oxygen.
4. Bronchodilator Testing
Sometimes spirometry is repeated after you inhale a medication that opens your airways. This helps your doctor see whether your breathing improves with treatment, which can be useful in evaluating asthma and other obstructive lung conditions.
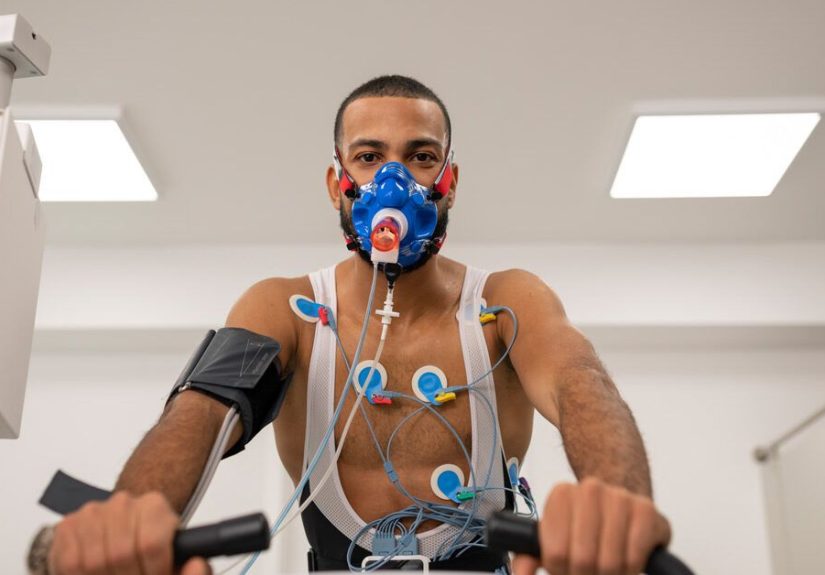
5. Cardiopulmonary Exercise Testing
Not every patient needs this one, but it can be very helpful when shortness of breath is complicated. During this test, you exercise on a bike or treadmill while your heart, lungs, and oxygen levels are monitored. It helps determine whether symptoms are coming mainly from the lungs, the heart, poor conditioning, or a mix of factors.
Why Would You Need a Pulmonary Function Test?
The purpose of a pulmonary function test is broader than many people realize. It is not just a test for people who already have lung disease. It can also help detect problems early, measure severity, and monitor changes over time.
Your provider may order lung function tests to:
- Evaluate symptoms such as cough, wheezing, chest tightness, or shortness of breath
- Help diagnose conditions like asthma, COPD, emphysema, pulmonary fibrosis, and some neuromuscular disorders
- Monitor an existing lung disease and see whether treatment is working
- Check lung health before surgery
- Assess the effects of smoking or environmental and workplace exposures
- Investigate whether medications or certain diseases are affecting the lungs
- Help explain exercise intolerance or unexplained breathing complaints
For example, if someone has a chronic cough that has outstayed its welcome by several months, spirometry can help determine whether the issue looks more like asthma or another airflow problem. If another person has progressive shortness of breath and abnormal imaging, lung volumes and diffusion testing may help show whether the pattern is restrictive, which can point toward scarring or stiffness in the lungs. And if a patient is preparing for a major operation, pulmonary testing may help estimate how well they can tolerate the procedure.
How to Prepare for a Pulmonary Function Test
Preparation is usually simple, but it matters. A surprisingly good breathing effort on test day is helpful. A cheeseburger the size of a bowling ball, less helpful.
Your testing center may give you specific instructions, but common preparation tips include:
- Wear loose, comfortable clothing
- Avoid a heavy meal for at least a couple of hours before the test
- Avoid smoking before the test, often for several hours or the full day
- Avoid heavy exercise shortly before testing
- Avoid alcohol for several hours beforehand
- Avoid caffeine if your testing center tells you to
- Ask whether you need to hold any inhalers or breathing medicines before the test
- Bring your glasses, oxygen, or medication list if instructed
If you wear dentures, many labs actually want you to keep them in because they can help you seal your lips around the mouthpiece. If you are claustrophobic, mention that before body plethysmography. If you have a cold, flu-like illness, recent surgery, or a recent heart problem, tell the testing center in advance. That information can affect whether the test should be done that day or postponed.
What Happens During the Procedure?
The exact procedure depends on which pulmonary function tests your provider ordered, but most appointments follow a similar pattern.
Before the Test
A technician or respiratory therapist usually records your height, weight, age, and other details used to compare your breathing results with expected reference values. Then you will get instructions for each test. The coaching part is important because good technique leads to more accurate results.
During Spirometry
You will sit upright, wear a soft clip on your nose, and place your mouth tightly around the mouthpiece. Then you will be asked to take your deepest breath in and blast the air out as hard and fast as possible. Most people repeat this maneuver at least three times so the results can be checked for consistency.
This part can feel surprisingly athletic. It is less “gentle yoga breath” and more “blow out the candles on a cake the size of a dining room table.” Some people cough during or after the effort. That is common.
During Body Plethysmography
You sit inside a clear booth and breathe through a mouthpiece while the machine measures pressure changes. The technician will guide you through shallow and deeper breaths. The booth is enclosed, but it is transparent, and the test is usually short. If closed spaces make you uncomfortable, speaking up early helps.
During a Diffusion Test
You breathe in a special gas mixture, hold your breath for several seconds, and then exhale. The machine measures how much gas was absorbed. This helps estimate how well gases move across your lung membranes into your blood.
During Exercise Testing
If exercise testing is ordered, you may walk on a treadmill or pedal a stationary bike while connected to monitoring equipment. The goal is not to win a race. The goal is to see how your lungs and heart respond to increasing physical effort in a controlled environment.
How Long Does a Pulmonary Function Test Take?
A basic spirometry visit may be fairly quick, but a full pulmonary function evaluation can take longer. The total time depends on which tests are included, whether bronchodilator testing is added, and how many rest breaks you need. In general, expect somewhere between about 30 minutes and 90 minutes. If you are tired during testing, tell the staff. Breaks are allowed.
What Do the Results Show?
Pulmonary function test results help providers understand the pattern of breathing impairment, but they do not always hand over a neat diagnosis with a bow on top. Instead, the results are interpreted along with your symptoms, exam findings, imaging, and medical history.
Broadly, results may suggest:
Obstructive Pattern
This means air has trouble moving out of the lungs efficiently. Obstructive patterns are common in asthma, COPD, and emphysema.
Restrictive Pattern
This means the lungs cannot fully expand or do not hold as much air as expected. Restrictive patterns may occur in interstitial lung disease, chest wall disorders, some neuromuscular conditions, or other causes of limited lung expansion.
Reduced Diffusion Capacity
This can suggest problems with gas transfer, which may happen with emphysema, pulmonary vascular disease, or certain forms of scarring and inflammation in the lungs.
Your provider may also look at whether your breathing improves after a bronchodilator, whether your results change over time, and how severe any abnormality appears compared with normal reference ranges.
Is a Pulmonary Function Test Painful?
Usually, no. Pulmonary function tests are noninvasive and not considered painful. There are no incisions, no needles for standard testing, and no dramatic movie soundtrack. That said, the effort can feel intense. Some people describe spirometry as tiring, awkward, or briefly uncomfortable because you have to inhale deeply and exhale forcefully on command.
Body plethysmography can feel cramped if you dislike enclosed spaces. Diffusion testing may feel a little strange because of the breath-hold. Exercise testing can be physically demanding, but it is supervised and designed around your tolerance.
Risks and Safety Concerns
For most people, pulmonary function testing is very safe. Still, “very safe” is not the same thing as “zero things can ever happen,” so it is smart to know the main risks and cautions.
Common Temporary Side Effects
- Lightheadedness or dizziness from repeated deep breathing
- Coughing during or after forceful exhalation
- Temporary fatigue
- Nervousness in a small booth during lung volume testing
- A faster heart rate during intense effort or exercise testing
These effects usually go away quickly once the test stops and you rest.
Rare but More Serious Risks
Serious complications are uncommon, but providers still screen for them. In rare cases, forceful breathing maneuvers may trigger chest discomfort or, very rarely, a collapsed lung. Exercise-based testing has more important safety rules because it places greater demand on the heart and lungs.
When Testing May Be Delayed or Avoided
Your provider may postpone or reconsider testing if you have had a recent heart attack, unstable chest pain, a current pneumothorax, a recent eye, chest, or abdominal surgery, or certain aneurysms. Acute respiratory infections may also be a reason to delay testing, especially when there is concern about accuracy or infection control. This is one reason you should always mention recent illness, surgery, or heart problems before the procedure.
Who Performs Pulmonary Function Tests?
These tests are usually performed by trained respiratory therapists or pulmonary function technicians in a clinic, outpatient lab, or hospital setting. The quality of the test depends heavily on good coaching and patient effort. In other words, you are not just breathing into a machine; you are doing a coached performance with data attached.
Tips for Getting the Most Accurate Results
- Follow medication instructions exactly
- Arrive on time so you are not rushed
- Wear clothes that let your chest and abdomen move freely
- Tell the technician if you feel dizzy, tired, or anxious
- Ask for the instructions to be repeated if anything is unclear
- Give your best effort, especially during spirometry
Even very sick patients can often complete pulmonary function testing with proper coaching and rest breaks. The goal is not perfection on the first try. The goal is reliable effort so the results actually mean something.
Experiences Related to Pulmonary Function Testing
For many patients, the biggest surprise is that a pulmonary function test feels more like a coached breathing workout than a traditional medical exam. People often walk in expecting something passive, like an X-ray, and then discover they are going to be asked to inhale deeply, exhale forcefully, repeat the effort several times, and follow instructions with game-show precision. That mismatch between expectation and reality is common.
A patient with possible asthma, for example, may come in because of nighttime cough and wheezing. During spirometry, they may feel fine at rest but notice that the forced exhalation makes them cough. That does not necessarily mean something is wrong with the test. In fact, coughing during spirometry is common, especially in people with sensitive or irritated airways. What matters is that the technician helps them repeat the maneuver correctly so the provider can see whether airflow is reduced and whether it improves after a bronchodilator.
Another common experience involves body plethysmography. Patients often say the clear booth looks intimidating at first, especially if they are prone to claustrophobia. In practice, many people find it easier than expected because the booth is transparent, the staff remains in view, and the test is short. The most uncomfortable part is often not the booth itself but the odd sensation of breathing through a mouthpiece while following precise instructions. It feels unusual, not painful.
People having diffusion testing sometimes describe it as the “hold your breath and do not mess this up” portion of the appointment. You take in a breath of test gas, pause for several seconds, and exhale on command. Most patients tolerate it well, but it can take a round or two to get the timing right. That is normal. Pulmonary testing is effort-dependent, and the technician’s coaching makes a major difference.
Patients who live with chronic lung disease often have a different perspective. For them, pulmonary function tests become a way to track progress over time. Someone with COPD may not love the effort involved, but they may appreciate seeing whether treatment is helping or whether their breathing is declining more slowly than before. A person with interstitial lung disease may feel anxious waiting for the results because the numbers help guide next steps. In that setting, the test is not just a one-time event. It becomes part of the story of the disease.
There is also the experience of relief. Many people are nervous beforehand because the name sounds serious. Then the test ends, they sit up, remove the nose clip, and realize it was manageable. They may feel briefly lightheaded, tired, or cough a little, but most return to normal activities soon afterward. The overall experience is often less dramatic than the imagination makes it. In medicine, that is a rare and beautiful gift.
Conclusion
A pulmonary function test is one of the most useful tools for evaluating breathing problems because it gives objective information about how the lungs move air and transfer oxygen. Whether the issue is asthma, COPD, unexplained shortness of breath, a pre-surgery check, or follow-up for known lung disease, PFTs help providers move from guesswork to evidence. The procedure may feel effortful, but it is usually safe, noninvasive, and completed in a single visit. If you know the purpose, understand the procedure, and prepare correctly, the test becomes much less intimidating and a lot more useful.





