Table of Contents >> Show >> Hide
- What Radiation Therapy Actually Does in Multiple Myeloma
- When Doctors Use Radiation Therapy for Multiple Myeloma
- How Radiation Therapy Is Usually Given
- Benefits of Radiation Therapy in Myeloma Care
- Limits and Trade-Offs Patients Should Understand
- Common Side Effects of Radiation Therapy
- How Radiation Fits With Other Multiple Myeloma Treatments
- Questions Patients May Want to Ask Their Care Team
- Final Thoughts
- Real-World Experiences With Radiation Therapy for Multiple Myeloma
When people hear the word “radiation,” they often imagine it as a headline treatment that marches in, conquers the cancer, and exits in a dramatic cloud of medical authority. Multiple myeloma, however, prefers to make things more complicated. This is a blood cancer that usually affects many areas of the bone marrow at once, so the main treatment plan often leans on systemic therapies such as drug combinations, targeted treatments, immunotherapy, and stem cell transplant strategies. Radiation therapy still matters a great deal, but it usually plays a more focused role. Think of it less as the whole orchestra and more as the star soloist brought in when one painful, dangerous, or stubborn spot needs immediate attention.
That targeted role is exactly why radiation therapy remains an important part of modern multiple myeloma treatment. It can shrink a plasmacytoma, calm severe bone pain, help control disease in a specific area, and protect function when the spine or nerves are under pressure. In the right setting, it can make a dramatic difference in how someone feels and functions. And in a disease where quality of life matters as much as lab numbers, that is no small thing.
What Radiation Therapy Actually Does in Multiple Myeloma
Multiple myeloma begins in plasma cells, a type of white blood cell found in bone marrow. When these cells become cancerous, they can crowd out healthy blood-forming cells and trigger damage in bones. That is why many people with myeloma deal with bone pain, lytic lesions, fractures, fatigue, anemia, and weakness. Radiation therapy works by directing high-energy beams at a specific target to damage cancer cells and stop them from multiplying.
In myeloma care, radiation therapy is usually not used to treat the whole disease throughout the body. Instead, it is used locally, meaning it targets a defined problem area. This distinction matters. If systemic therapy is the full-house cleaning crew, radiation is the specialist brought in to deal with the one room that is on fire.
That focused design is part of its strength. It allows doctors to treat a painful or risky lesion without automatically changing the entire treatment strategy. It can also be layered into a broader plan that includes anti-myeloma drugs, bone-strengthening medicine, surgery, or rehabilitation support.
When Doctors Use Radiation Therapy for Multiple Myeloma
1. Painful Bone Lesions That Are Not Behaving
Bone pain is one of the most common and frustrating symptoms of multiple myeloma. It can show up in the back, ribs, hips, arms, or legs, and it does not exactly ask permission before interfering with sleep, walking, or basic daily life. When pain medicines, systemic therapy, or supportive care are not doing enough, radiation can be used to shrink the local myeloma growth causing the trouble.
This is one of the best-known uses of radiation in myeloma. For many patients, the goal is palliative, but that word should not be confused with “minor.” Palliative treatment can be powerful. If a few focused sessions mean a person can stand up without wincing, get out of bed more easily, or stop planning the day around pain spikes, that is a meaningful win.
2. Areas of Bone That May Be Near Breaking
Myeloma can weaken bones enough to create a real risk of fracture. When imaging shows a damaged area that is unstable or nearly unstable, radiation may be used as part of the strategy to control the lesion and reduce further destruction. In some cases, it is combined with orthopedic procedures, braces, or surgical stabilization. That is because cancer care loves a team effort, especially when the skeleton has started filing formal complaints.
3. Spinal Cord Compression or Nerve Pressure
This is the big one. If myeloma damages vertebrae in the spine, those bones can collapse or shift in a way that presses on the spinal cord or nearby nerves. This can cause severe pain, weakness, numbness, trouble walking, or changes in bowel and bladder function. It is considered a medical emergency.
In this setting, radiation therapy may be used quickly to reduce the tumor burden and help relieve pressure, often alongside steroids, surgery, or both. The message here is simple: if someone with myeloma develops sudden new weakness, numbness, or loss of control over urination or bowel movements, that is not a “let’s mention it at the next appointment” moment. That is an urgent call to the cancer team or emergency care.
4. Solitary Plasmacytoma
Radiation has a special place in the treatment of solitary plasmacytoma, a single collection of abnormal plasma cells in one bone or one soft-tissue site. Unlike classic multiple myeloma, this is a localized plasma cell tumor. In that setting, radiation therapy may be used with curative intent because the disease is confined to one area.
That does not mean the story always ends there. Even after successful treatment, careful long-term follow-up is still needed because some people eventually develop multiple myeloma later on. Still, this is one of the clearest examples of radiation stepping out of the supporting role and taking center stage.
How Radiation Therapy Is Usually Given
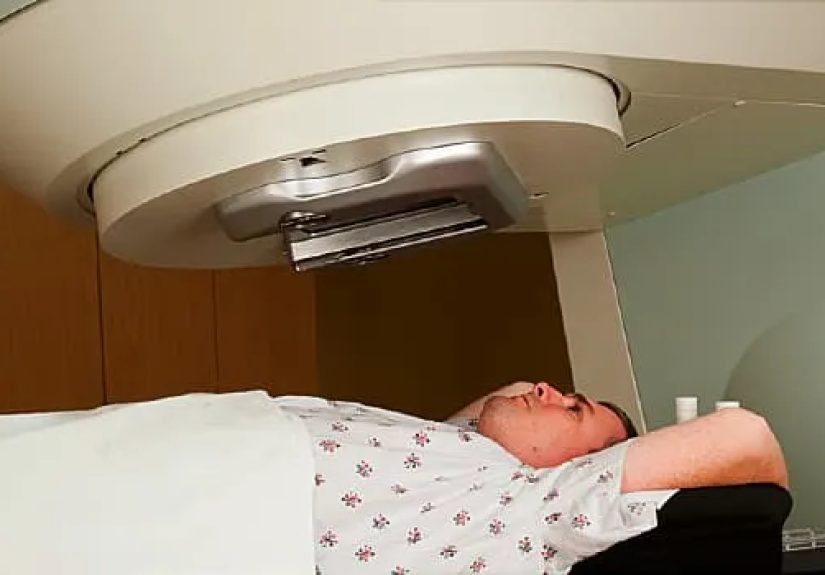
For myeloma and plasmacytoma, the most common approach is external beam radiation therapy. That means the radiation comes from a machine outside the body and is aimed precisely at the treatment area. Before treatment starts, patients usually have a planning visit called simulation. During this step, the team maps the exact target using imaging and positioning tools so the dose goes where it is needed while limiting exposure to nearby healthy tissue.
Actual treatment sessions are usually short. The setup often takes longer than the radiation delivery itself. Patients do not feel the beam while it is happening, which can be both reassuring and weirdly anticlimactic. Many people go in expecting to feel something dramatic and instead discover that the machine does all the work while they lie still and try not to become suddenly interested in scratching their nose.
The schedule depends on the treatment goal, the size and location of the lesion, nearby normal tissues, and how the rest of the myeloma plan is being coordinated. Some people receive a short course over just a few visits, while others may need a longer schedule. The radiation oncologist and hematologist usually work together to time treatment around systemic therapy, especially when bone marrow function is already under strain.
Benefits of Radiation Therapy in Myeloma Care
The biggest benefit is straightforward: radiation can work quickly and locally. It can reduce pain, shrink a troublesome mass, and help stabilize a dangerous situation. In many cases, it improves mobility, sleep, and day-to-day comfort. That matters because myeloma treatment is often a marathon, and anything that makes the marathon more livable is clinically important.
Another advantage is precision. Modern radiation techniques can shape treatment closely around the target. That allows doctors to treat difficult areas while trying to spare healthy tissues as much as possible. Precision does not make radiation trivial, but it does make it more manageable and more compatible with the larger treatment plan.
Radiation can also fill an important timing gap. Systemic therapies may take time to fully control disease, while a specific painful lesion or compressive mass may need attention now. Radiation is often the answer to that “now” problem.
Limits and Trade-Offs Patients Should Understand
Radiation therapy is useful, but it is not a magic wand. Because multiple myeloma is usually a systemic disease, local radiation does not replace whole-body treatment strategies. A painful rib lesion may improve, but that does not mean the disease elsewhere has been solved. This is why radiation is commonly one tool in a much larger kit.
Another key issue is bone marrow. Myeloma already affects marrow function, and many treatments used for the disease can lower blood counts. Radiation, especially when larger areas are treated, can add to that burden. This is one reason doctors think carefully about dose, field size, and timing. The goal is not merely to treat the lesion but to do it in a way that does not create unnecessary downstream trouble for the rest of the plan.
There is also a practical reality: pain relief may not be instant. Some people feel better fairly soon, while others improve more gradually over days or weeks. Managing expectations helps. Radiation is a powerful tool, but it is still biology, not a light switch.
Common Side Effects of Radiation Therapy
Side effects depend heavily on where the radiation is aimed. That is why one person might mainly feel tired while another develops nausea, bowel changes, or irritation in the treated area. The most common issues are often temporary, but “temporary” can still feel very real when you are the one living through it.
Side effects that may occur include:
- Fatigue that builds gradually during treatment
- Skin changes in the treated area, such as redness, dryness, peeling, or tenderness
- Nausea if the treatment area is near the abdomen
- Diarrhea if the pelvis or belly is treated
- Low blood counts, especially in people whose marrow reserve is already limited
- A temporary pain flare in the treated bone before relief sets in
Most side effects improve after treatment ends, but patients should not try to “tough it out” in silence. Radiation teams are very used to helping manage side effects. In oncology, pretending everything is fine rarely earns a medal, and it definitely does not improve skin irritation.
How Radiation Fits With Other Multiple Myeloma Treatments
Radiation is only one chapter in the broader myeloma story. Depending on the stage and behavior of the disease, patients may also receive combinations of steroids, proteasome inhibitors, immunomodulatory drugs, monoclonal antibodies, bispecific therapies, CAR T-cell therapy, chemotherapy, bone-modifying agents, and transplant-based approaches. The exact lineup depends on whether the disease is newly diagnosed, relapsed, refractory, localized, or associated with complications.
That is why treatment planning needs coordination. A radiation oncologist focuses on the local problem, while the hematologist or myeloma specialist manages the bigger disease picture. Orthopedic surgeons, neurosurgeons, palliative care clinicians, rehabilitation specialists, and pain teams may also be involved. The best myeloma care often looks less like a solo performance and more like an extremely organized group project.
Questions Patients May Want to Ask Their Care Team
- What is the main goal of radiation in my case: pain relief, tumor control, nerve protection, or treatment of a plasmacytoma?
- How many treatments are planned, and over what time period?
- How will radiation affect my blood counts?
- When should I expect pain relief?
- Could I have a temporary pain flare first?
- How will radiation fit around my systemic therapy schedule?
- What side effects are most likely based on the area being treated?
- What symptoms should prompt me to call right away?
Final Thoughts
Radiation therapy for multiple myeloma treatment is not usually the main event, but it is often one of the most useful supporting players on the stage. It can ease stubborn pain, shrink dangerous or disruptive tumors, protect the spinal cord, and serve as a primary treatment for solitary plasmacytoma. In other words, it may not treat every myeloma cell in the body, but it can make a huge difference in the place that is currently causing the most trouble.
If you or someone you love is facing radiation as part of a myeloma plan, the smartest mindset is focused curiosity. Know why it is being recommended, what problem it is trying to solve, how it fits with the rest of treatment, and what side effects to watch for. Radiation is at its best when it is used strategically, not mysteriously. And honestly, that is true for almost everything in cancer care.
Real-World Experiences With Radiation Therapy for Multiple Myeloma
One of the most useful things to understand about radiation therapy is that the lived experience is often less dramatic than the name suggests and more emotionally layered than the schedule on paper. Patients commonly describe a strange mix of relief and frustration. Relief, because radiation is often offered for a very specific problem such as severe pain, a growing plasmacytoma, or pressure on a nerve. Frustration, because by the time radiation enters the picture, life may already have been disrupted by scans, clinic visits, fatigue, and the general annoyance of having a cancer that does not respect calendars.
For many people, the first surprise is how technical and carefully choreographed the process feels. The planning appointment can make treatment seem serious in a very concrete way. The team marks the target, explains positioning, and emphasizes staying still. It is not painful, but it can make the whole thing suddenly feel real. Some patients say the machine looks intimidating, while the actual session feels almost anticlimactic. You lie there, hear the machine move, feel nothing from the beam itself, and then it is over. For newcomers, that gap between how big it sounds and how quiet it feels can be oddly reassuring.
Pain relief is another area where experience varies. Some people notice improvement fairly soon and describe the change almost like getting part of their life back. Sleeping becomes easier. Walking hurts less. A favorite chair stops feeling like an enemy. Others improve more gradually and need patience, which is not exactly the easiest emotion to order on demand. A temporary pain flare can also throw people off because it feels backwards. If that possibility is explained ahead of time, it is easier to manage. If it is not, patients may worry the treatment is failing when it may simply be too early to judge.
Fatigue is one of the most commonly described side effects, but people often say it is a sneaky kind of tiredness. It is not always the theatrical collapse people expect. Instead, it can feel like the day shrinks. Tasks take longer. Motivation goes on vacation without notice. Even small errands start negotiating for their own lunch break. For patients who are also receiving systemic therapy, it can be hard to tell which treatment is causing what, and that uncertainty is part of the experience too.
Caregivers often have their own version of the radiation journey. They become drivers, note takers, snack carriers, symptom watchers, and unofficial morale staff. Many say the routine of daily appointments creates structure, which can be comforting, but also exhausting. The emotional load is real: everyone wants the treatment to work, and no one loves waiting for proof.
There is also the psychological effect of targeted treatment. Patients frequently say that radiation feels purposeful because it is aimed at a known problem. In a disease as complicated as multiple myeloma, that clarity can be grounding. When a scan shows one lesion causing major trouble, and the team has a direct plan for that exact spot, it can restore a sense of control. It may not solve everything, but it solves something, and sometimes that is exactly what people need most in the moment.




![“[Am I The Jerk] For Telling My Wife I’m Not Going To Sacrifice My Hobbies Just So That I Can Babysit?”](https://2quotes.net/wp-content/uploads/2026/04/am-i-the-jerk-for-telling-my-wife-im-not-going-to-sacrifice-my-hobbies-just-so-that-i-can-babysit-iqoh9o4a-thumb.jpg)